Periodontics
Periodontics is the area of Dentistry that is responsible for the study, prevention and treatment of those pathologies that affect the tissues that protect, surround and support the teeth: gums, alveolar bone, periodontal ligament and root cement.
Periodontal lesions are produced by the accumulation of bacteria, which cause alterations of the periodontium. If they are not treated, these ailments progress progressively, and can cause tooth loss and various conditions in our body.
El colégio de odontólogos ha creado una pagina con información para mejorar la salud de tus encías. Para más información haz click aquí
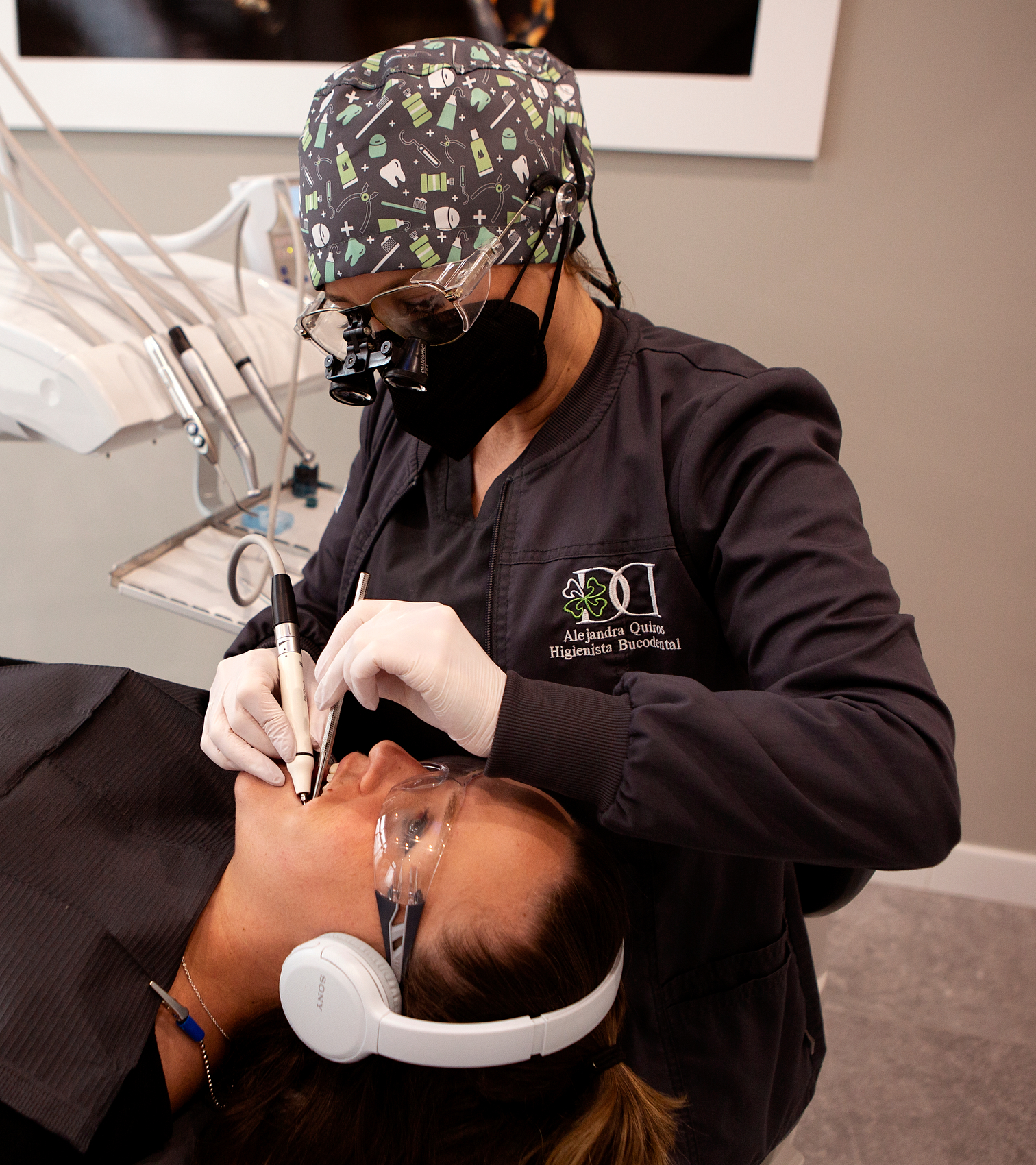
Periodontal disease
Periodontal disease is a chronic pathology, which includes outbreaks with minimal symptoms and can lead to the loss of support for the teeth, that is, to the destruction of the gums and the bone that support the teeth.
Better dental training in the field of prevention, as well as greater awareness and education of society about what periodontal disease is and basic oral hygiene measures are considered essential to prevent periodontal pathologies and curb the growing problem they pose these illnesses.
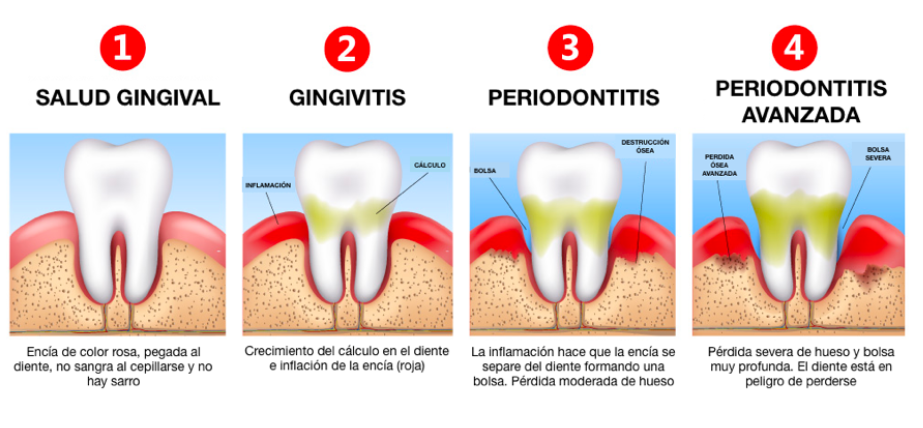
There are two types of periodontal diseases.
Gingivitis. Initial phase of periodontal disease, which is caused by the accumulation of bacterial plaque, made up of bacteria and debris that adhere to the teeth. If it is not removed correctly, it turns into tartar, which irritates and inflames the gums. The most common symptoms are redness in the area and bleeding gums. Gingivitis is a reversible condition, but if not treated properly, it can progress to periodontitis.
Periodontitis. It is a serious and irreversible periodontal disease, which affects between 15% and 20% of adults between the ages of 35 and 44, according to the World Health Organization. This pathology, unlike gingivitis, is characterized by the structural loss of the attachment apparatus. Periodontitis is the main reason for dental loss in adults.
IN RECENT YEARS, several new and important aspects have been developed in the field of prevention and management of periodontal diseases.
What’s new?
One of the main innovations derives from a new classification of periodontal disease, which focuses on following all phases of periodontal treatment and achieving the motivation of the patient as an active part during treatment.
Substantial progress has also been made in the identification and control of the main risk factors associated with the appearance and development of periodontal disease (tobacco, diabetes…).
Fundamentally, the considerable increase in research and clinical evidence linking oral health with general health, even demonstrating how an optimal treatment of periodontitis has a positive systemic impact on other parts of the body and a benefit beyond the oral cavity. highlighting the relationship between periodontal diseases with systemic diseases (such as diabetes, some cardiovascular diseases, rheumatoid arthritis or Alzheimer’s).
All this has gone hand in hand with a substantial change in the role of the periodontist-dentist, who is currently also involved in the task of achieving good general health for the patient.

-
1st Phase:
a) Teach the patient to control plaque formation (with motivation and personalized oral hygiene instructions) and risk factors (smoking cessation, better diabetes control…). Biofilm control must be mechanical (manual or electrical brushing and interdental cleaning) and with chemical means (dentifrices and antiseptic mouthwashes).
b) Elimination of supragingival calculus (visible) and local retention factors by the professional.
-
2nd Phase
Treatment directed at the cause is started, eliminating the subgingival biofilm (not visible as it is located under the gum) and the calculus by means of subgingival instrumentation (scaling with curettes or sonic or ultrasonic instruments) and which may be accompanied by the use of antimicrobial agents.
Subsequently, a reassessment of the response of the periodontal tissues to the periodontal treatment performed should be carried out. If periodontal health has been achieved, it will go on to the maintenance phase; If deep periodontal pockets persist, further scaling, periodontal surgery, or dental extractions should be considered.
-
3rd Phase
In areas with residual pockets, a new scraping is performed (if they are less than 4-5 mm), if they are deeper (more than 6 mm), access periodontal surgery is recommended.
-
4th Phase
When the patient’s periodontal stability has been achieved, patients should start the periodontal maintenance program.
Periodontal maintenance is preventive and therapeutic: systemic and periodontal health monitoring, reinforcement of personalized oral hygiene instructions, patient motivation to control risk factors, plaque removal and subgingival professional calculation of residual pockets.
Maintenance is recommended at intervals of 3-6 months, depending on the patient’s risk and bone loss.
Periodontitis must be treated correctly, following four phases and finishing periodic periodontal maintenance for life.
From gum health to general health
The mouth is not isolated in the body, but is intimately linked to the body in general. Inflammation is not confined to the periodontal tissues, but the bacteria that cause periodontitis and their endotoxins enter the bloodstream and spread systemically.
In recent years, associations have been found between periodontal disease and chronic diseases, such as cardiovascular, respiratory and kidney diseases, premature births, diabetes, rheumatoid arthritis, metabolic syndrome, cognitive impairment and cancer, highlighting the importance of good oral health. in prevention systemic consequences of periodontitis.
Based on this reality, dentists, as health professionals, are involved in achieving good general health for their patients, so it is essential in their work to promote good nutrition, physical activity, stress reduction or the cessation of of the smoking habit.
And don’t forget…
Implementing a complete periodontal treatment and maintaining periodontal health is essential to carry out a successful interdisciplinary treatment in the future.